Maintaining mental activity and social contact are life savers according to Public Health England, as social isolation is a killer condition linked to 30% increase in death. It is not just mental health that is affected but physical health too. This was one of the key messages from a recent conference of health and social care experts in Cambridge which was memorably introduced by TV presenter Jennie Bond. She advocated taking on challenges in later life and gave examples of her risk-taking, from starting to run regularly, practising balance by teeth brushing on one leg, to more extreme pursuits like the bush-tucker challenge in the “I’m a celebrity” jungle. The topics explored in the conference ranged from how buildings and town planning can help older people through technology to nursing working practices that empower people & carers to manage health more independently.
Building a better world
One of the simplest improvements to the built environment to combat social isolation is the provision of public toilets, benches and green spaces.

Prof Sarah Wigglesworth explained that it is common for older people to need the loo more often and to become tired more quickly than young people. When people are anxious about finding a loo or a comfortable place to rest when they need it, they tend to go out less frequently to the point when crossing the threshold becomes an unfamiliar, daunting challenge and they are confined to their home. So public loos are good for our health and wellbeing – not rocket science, but not immediately obvious until the factors that cause social isolation are thought through.
A theme that recurred was that as we are living longer we can improve things for ourselves by planning for common changes, including down-sizing to a home which can be comfortably managed.
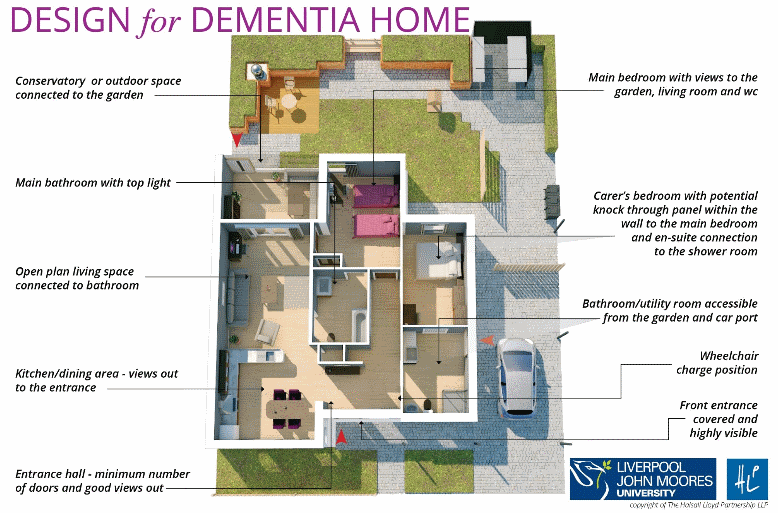
Smaller doesn’t have to mean lower quality and Chris Marsh from the Building Research Establishment showed flat layouts that have been created for older people: wide entrance and corridors, glazed doors & open spaces to aid orientation, a loo in the centre of the property so it is easily accessible and two bedrooms so friends and family can stay – or a live-in carer if that is appropriate. Details even include the types of materials used in walls so sound does not travel while valued Wi-Fi and mobile signals do. Conversely, poor quality homes have been estimated to cost the NHS £1.4bn a year due to preventable trips and falls.
Harness Technology
In the panel discussion on how technology will impact ageing, views were shared from the conservative to the radical. Common ground was expressed by Dr Jenni Lynch that there is no shortage of technology, but use has to be shaped by people’s needs and wishes – an approach called co-design and co-production. Prof Pat Schofield underlined this by pointing out that older people are not a homogenous group and while Wii Fit may encourage one person to exercise, it may put another off.
A problem with conventional computers, phones and tablets is that they require good eyesight & dexterity to use, yet these commonly decline with age – this is a barrier to technology adoption by older people. Paul Swift, the Digital programme manager for Age UK, said that voice-control offers a major opportunity to give people access to technology in an uncomplicated way. He referenced a group of octogenarians in the USA who use the Amazon Echo (reviewed here) to listen to audio books, keep current with family news, and control home appliances . Paul and team have already put AgeUK’s streaming radio station, the Wireless, on Alexa. Playing it is as simple as saying
“Alexa, play Wireless Radio.”
The topic that divided opinion was the use of robots in care. Particularly polarising was use of robots to reduce social isolation in the “CARESSES” project (Culture-Aware Robots and Environmental Sensor Systems for Elderly Support). As part of the presentation, this video was shown. In the following Q&A session it was clear that some were appalled by the idea of using a robot for example to help someone pray, pointing out that social interaction was the part of the job carers valued most. Others welcomed the innovative thinking by Prof Gurch Randhawa who described his work as having a moral imperative.

Chatting with delegates afterwards there was a feeling that a tablet or smart TV with some appropriate apps supplemented by voice-control may be more appropriate solutions to social isolation, helping preserve purpose with games, social media and video-chat to maintain social networks as well as access to entertainment and home control with voice command. Care workers can provide further social interaction while robots can in the future perform cleaning or lifting functions.
Combating learned helplessness – Buurtzorg – relationship-based care
One presentation that drew a lot of interest suggested that modern healthcare suffered from a command and control culture exemplified by atomisation and task orientation of care where a person with 2 chronic problems (a complex patient) can see 20+ different people in a normal week. This conveyor belt of unconnected carers (an oxymoron?) who come to treat an ailment but don’t know the individual, creates ‘learned helplessness’, where care is resigned to the busy experts. A team of community nurses in the Netherlands have established a new relationship-based approach to care called Buurtzorg – ‘neighbourhood care’ in Dutch. It has proved very successful, with lower costs and overheads and better prevention levels than conventional approaches. The key idea is to train and equip the service-user (patient) and importantly their informal care network to self-manage their care; this empowers them to take control and so preserves their purpose.
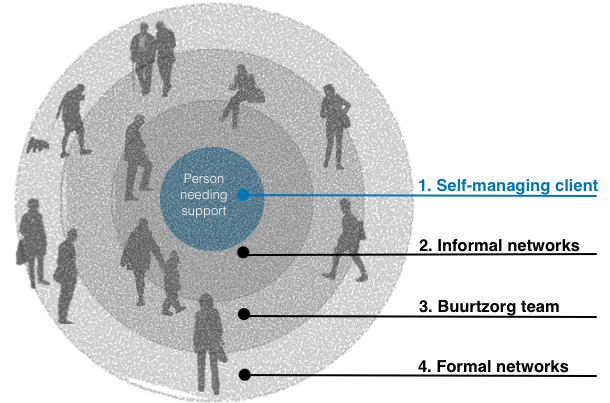
The Buurtzorg nurses organise the care plans, equip people and bring in specialist care when needed. Digital technology was described as important to this model along with an assessment method called the Omaha model. These provide a platform for sharing care information more consistently & easily, giving insight on the effectiveness of interventions as they and their outcomes are consistently described and recorded. The value these deliver are a reduction in bureaucracy, an increase in productivity and improved quality of care. All very impressive and spreading rapidly across the globe with the latest launch in Cambridgeshire.
The conference showed that while ageing brings change for people, it affects people in different ways and to different degrees. A long life means there is more time to plan, and this will become increasingly important as working life and diminished health are more likely to overlap. It is great to know that health and social care academics and professionals are anticipating these changes and are working to improve care by focussing on a personal approach and working out how modern technology can improve person-centred care, connect people to their social networks, empower them to self-manage their care and so through these preserve purpose.
—
A short video of the conference is here and the slides presented are here. Images used in this article are from the conference, ownership belongs to those mentioned in the text.
